Complete Guide to the Endocannabinoid System
Article written by

Tina MagrabiSenior Content Writer
Content reviewed by

Dr. Lewis JasseyMedical Director - Pediatric Medicine
Every person — and many animals — has an endocannabinoid system (ECS), a complex network of receptors, lipids, and enzymes that plays a significant role in regulating homeostasis and how we individually experience cannabis.
While the ECS was just identified in the late 1980s, it quickly became one of the most important scientific discoveries. The ECS plays a role in sleep, appetite, immune function, and virtually every critical life function. When the endocannabinoid system is out of balance, we are also off-kilter and not functioning optimally.
Endocannabinoid deficiencies often precede disease, so the system is dubbed the master regulator.
Get your medical marijuana card
Connect with a licensed physician online in minutes.
How the Endocannabinoid System Works
The ECS has three main parts: endocannabinoids, receptors, and enzymes.
Endocannabinoids
Cannabinoids are chemicals in cannabis (and many other plants) that interact with the ECS. Tetrahydrocannabinol (THC), the molecule known for its intoxicating effects, and cannabidiol (CBD), known for promoting relaxation, are some of the more well-known cannabinoids. Still, the cannabis plant contains over 150 different types of these chemicals.
In addition, the human body generates its version of cannabinoids that interact with other elements of the ECS, called endocannabinoids. Endocannabinoids are cannabinoids produced by the body, which bind to receptors found in immune cells, throughout the nervous system, up and down the spine, in every brain cell, and even in the skin.
Anandamide (AEA) and 2-Arachidonoylglycerol (2-AG) are primary endocannabinoids.
Anandamide is the human body’s naturally occurring THC. Anandamide was discovered in the 1990s and named after the Sanskrit word “ananda,” meaning eternal happiness — it interacts with the body similarly to THC, which induces euphoric highs in many individuals.
2-AG can have both pain-killing and anti-inflammatory effects. 2-AG is present in the central nervous system (CNS) at relatively high levels.
Receptors
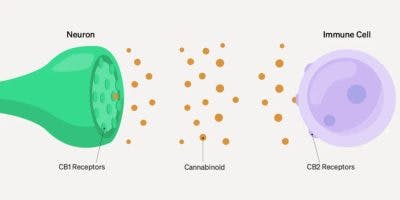
Cannabinoid receptors are crucial to the body’s endocannabinoid system (ECS). Every human body must maintain homeostasis, and cannabinoid receptors are the sites that — when activated — play a role in achieving this balance.
Cannabis works on cannabinoid receptors to exert different effects, many of which may provide therapeutic benefits.
What Are Cannabinoid Receptors?
Cannabinoid receptors exist throughout the body, including the brain, organs, glands, connective tissues, and immune cells. These receptors are thought to be more numerous than any other kind of receptor. When stimulated, cannabinoid receptors set off chain reactions responsible for various physiological responses, such as memory and immunity.
Science has identified two kinds of cannabinoid receptors:
- CB1 receptors are predominantly found in the brain and central nervous system, though they exist in various organs, glands, and other connective tissues. CB1 receptors are the main target of THC and anandamide, the body’s version of the cannabinoid. THC is an agonist of — or activates — the CB1 cannabinoid receptor, binding to it and producing the cannabinoid’s intoxicating effects.
- CB2 receptors are found primarily in the immune system and the peripheral nervous system, though some are also present in the brain. 2-AG, another endocannabinoid, and THC mainly act on these receptors.
Many body parts contain CB1 and CB2 receptors, each responsible for different physiological processes.
How Cannabinoid Receptors Help the Body
A well-functioning endocannabinoid system is essential for health, and cannabinoid receptors make the whole system run. Endocannabinoids and cannabinoids either activate or block the activation of CB1 and CB2 receptors, resulting in various discernible effects.
Pain Relief
Cannabis acts on cannabinoid receptors to help relieve aches and pains in the body in two significant ways.
First, the cannabinoid tetrahydrocannabinol (THC) interacts with pain receptors in the brain, diminishing the sensation of pain and improving the quality of life for people with conditions such as multiple sclerosis (MS) or chronic pain. Second, cannabidiol (CBD) acts on the inflammatory response system, helping block cytotoxins that cause inflammation and reduce painful sensations.
Anxiety Reduction
Cannabinoid receptors also play a role in regulating mood and energy levels. Using cannabis, one can soothe anxiety and cope with insomnia or other sleep disorders thanks to the cannabinoid receptors involved in our sleep cycles.
Appetite Regulation
CB1 and CB2 receptors play a role in appetite regulation and diet, making cannabis helpful in stimulating appetite and helping to regulate insulin. While THC can cause the munchies, which may be beneficial for those with diminished appetites, CBD can suppress feelings of hunger to manage caloric intake.
Neuroprotective Properties
Given the density of CB1 receptors in the brain, it makes sense that the stimulation of these neurons helps protect them and may prevent degenerative diseases. THC has been demonstrated to boost brain health, while CBD reportedly has neuroprotective properties.
How Cannabis Interacts with Cannabinoid Receptors
The different chemicals in cannabis interact with cannabinoid receptors in specific ways, with various quantities producing individual nuanced experiences.
Again, THC — the most prevalent cannabinoid in marijuana — acts on CB1 and CB2 receptors, binding at the sites to stimulate different physiological activities. THC stays in your system until it is eventually metabolized by the body, with higher amounts making the effects last longer.
CBD, the second-most common cannabinoid, is not an agonist and does not bind with cannabinoid receptors. Instead, it acts as an antagonist at CB1 receptors and blocks the uptake of agonists (either THC, endocannabinoids, or other chemicals). CBD inhibits CB1 receptors and limits their activities, preventing overzealous immune responses such as pain or inflammation and counteracting some of the effects of THC.
Enzymes
The third component of the endocannabinoid system is enzymes that metabolize and break down cannabinoids and endocannabinoids. Two primary enzymes include fatty acid amide hydrolase (FAAH), which breaks down anandamide and THC, and monoacylglycerol lipase (MAGL), which eliminates 2-AG.
These prevent dangerous endocannabinoids and phytocannabinoids from building up in the body. And yes, the levels of these cannabinoids can be hazardous because the ECS is all about achieving the right balance.
What Does the ECS Do?
A better question might be, what does the endocannabinoid system not do? The ECS is involved in regulating many of life’s most essential processes, including:
- Reward perception.
- Reproduction.
- Inflammatory response.
- Immune system function.
- Appetite.
- Pain sensation.
- Mood.
- Memory.
- The pleasurable effects of exercise.
- And, of course, mediating the pharmacological and experiential impact of cannabis.
In short, the ECS does a lot more than you might think!
Phytocannabinoids and the Endocannabinoid System
Phytocannabinoids are cannabinoids that the cannabis plant produces. To exert different effects, they bind to endocannabinoids, which your body naturally creates. Two of the most prominent phytocannabinoids in cannabis are THC and CBD.
THC
THC is an effective painkiller and could also be helpful as an anti-inflammatory, treatment of spasticity, nausea/vomiting, preventative therapy, appetite stimulant, and treatment for an overactive bladder.
CBD
CBD may be beneficial as an anti-inflammatory, mood stabilizer, and antispasmodic. This can make CBD helpful for managing chronic pain, anxiety and depression, multiple sclerosis, and epilepsy.
Other Phytocannabinoids
THC and CBD are just the beginning of the phytocannabinoids that the cannabis plant produces. Other phytocannabinoids like cannabichromene (CBC), cannabigerol (CBG), and cannabinol (CBN) all offer benefits. Tetrahydrocannabivarin (THCV) is another cannabinoid that has garnered lots of interest, and the terpene beta-caryophyllene is considered a dietary cannabinoid.
Foods with Phytocannabinoids
Enhance your endocannabinoid system by eating some of these tasty foods that contain phytocannabinoids:
- Chocolate.
- Veggies like kale and broccoli.
- Spices like cinnamon and black pepper.
Some of these foods, like black pepper, can help temper a negative experience with cannabis and get your ECS back on track.
What Is Clinical Endocannabinoid Deficiency (CED)?
Clinical endocannabinoid deficiency (CED) is a theory posited by Dr. Ethan Russo. Russo explains how many (but not necessarily all) medical conditions coincide with shortages, a dysregulation of the production, metabolism, and amount of endocannabinoids, or a change in the state or condition of cannabinoid receptors.
This disruption or deficit can come from an injury, infection, an event that triggers long-term inflammatory responses, or genetic dysfunction. Research has connected many medical conditions with a CED, including fibromyalgia, migraines, and irritable bowel disorders (IBDs). Chronic pain, insomnia, anxiety, and depression may also be linked to CED.
Furthermore, autoimmune disorders can cause widespread inflammation, and cannabinoids may help reduce this inflammation. Dravet and Lennox-Gastaut syndromes (two types of epilepsy) could arise due to the lack of genetic coding for a specific cannabinoid that helps regulate calcium and sodium ions.
In theory, one could have an overabundance of cannabinoids as well. A patient named Jo Cameron reportedly lacked the genetic code to produce the enzyme FAAH. This resulted in an overload of anandamide in her system, meaning she hardly felt any pain or anxiety. It is best to have neither deficiencies nor excesses in the ECS; balance is the key.
Can Long-Term Cannabis Use Affect the ECS?
There is insufficient evidence to understand how long-term use of cannabis may affect the ECS. Always err on the side of caution when using cannabis or any other drug and consume as directed by your physician.
How to Strengthen and Heal the ECS
In a word? Balance. The ECS is intimately involved in homeostasis — keeping the body’s physiological processes stable and balanced. You already have the tools to strengthen and heal your own ECS.
Here are a few simple ways to keep your ECS in top form:
- Get adequate sleep (seven to nine hours every night).
- Eat nutritious foods, especially those containing phytocannabinoids (decadent dark chocolate).
- Exercise, maintain a healthy weight, and spend time in the fresh air.
These basic lifestyle principles tremendously impact your general health and how good you feel daily.
See how medical marijuana can help boost your endocannabinoid system and apply for your MMJ card. The doctors at Leafwell are on-call to guide you through the application process and meet with you in our virtual clinic.
The Bottom Line
The endocannabinoid system (ECS) regulates vital physiological processes such as sleep, appetite, pain sensation, and mood. An imbalance, known as clinical endocannabinoid deficiency (CED), may contribute to various medical conditions.
Phytocannabinoids like THC and CBD interact with the ECS, offering therapeutic potential, though the long-term effects of cannabis on the ECS remain unclear.
Consulting healthcare professionals, like those at Leafwell, can provide guidance on medical marijuana use and obtaining a medical marijuana card for potential ECS regulation and greater overall well-being.
Get Your Medical Card
Connect with a licensed physician online in minutes.
Originally Published: November 2021
Last Updated: March 2024
Frequently Asked Questions
Is the endocannabinoid system real?
Yes, the endocannabinoid system is a real functioning system in your body. Many other mammals also have an ECS, including domestic cats and dogs, which is one reason why some veterinarians use CBD oil to treat certain conditions in pets.
Do our bodies produce cannabinoids?
Our bodies naturally produce endocannabinoids, which are cannabinoids made within our ECS. They interact with phytocannabinoids from the cannabis plant to have a synergistic effect.
How does CBD affect the endocannabinoid system?
CBD helps regulate the ECS in many ways, including a complementary natural treatment for depression and a tool to help manage pain.



